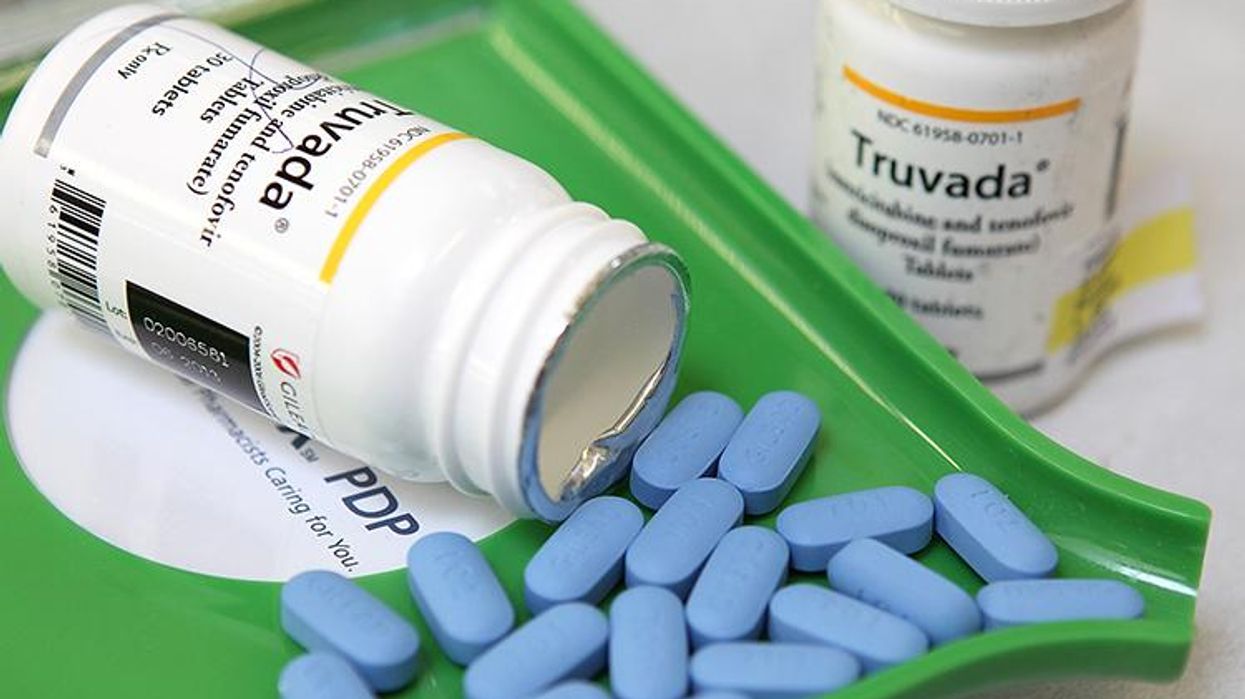
It's been nearly two years since the Centers for Disease Control and Prevention issued historic guidelines recommending that thousands of Americans -- particularly gay and bi men, transgender women, injection drug users, and partners of HIV-positive people -- start taking Truvada as pre-exposure prophylaxis (or PrEP) to prevent HIV infection.
The prevention method has shown to be 99 percent effective at preventing HIV transmission among those who take it daily as prescribed and, as was reported at the Conference on Retroviruses and Opportunistic Infections this week, it's even 86 percent effective among those using it "on demand" (essentially one dose two to 24 hours before sex, and then twice more the two days following sex).
Truvada as PrEP has had its critics from the get-go, notably Michael Weinstein, the head of AIDS Healthcare Foundation, who has led what some activists called a moral crusade against the drug. But many scientists, doctors, public health experts, and activists have heralded the prevention method as part of the necessary one-two punch needed to get HIV and AIDS numbers lowered in the U.S. (The other part is treatment as prevention--TasP -- in which people who are HIV-positive take medication to reach viral suppression so they can no longer transmit HIV to others). The CDC's own study, reported this week at CROI, in fact, says that PrEP has the potential to reduce new HIV infections by at least 70 percent in the United States.
But Weinstein and naysayers finally got the tiniest bit of ammunition in the culture war over PrEP. Researchers reported the first documented case of HIV infection this week of a man who appears to have been using the treatment regularly and as recommended. Dr. David C. Knox, a physician at Toronto's Maple Leaf Medical Clinic and the lead author of the study presented at CROI, says that a 43-year-old Canadian man is believed to have been taking PrEP for two years when he seroconverted to a multidrug-resistant strain of HIV, despite "clinical and pharmacokinetic data suggesting long-term adherence" to PrEP.
The man's virus was found to be resistant to multiple drugs, including emtricitabine and tenofovir, the two main ingredients in Truvada. When researchers from Maple Leaf, St. Michael's Hospital (also in Toronto), the British Columbia Centre for Excellence in HIV/AIDS in Vancouver, and the University of Colorado -- all coauthors of the CROI study -- did standard and deep sequencing of the virus from day 7, it revealed CCR5-tropic clade B HIV-1 with mutations conferring resistance to several classes of HIV drugs, nucleoside reverse transcriptase inhibitors, nonnucleoside reverse transcriptase inhibitors, and integrase inhibitors.
Phylogenetic analysis revealed a very narrow range of sequence diversity, consistent with infection from a single source, which led researchers to believe that the HIV was transmitted from a single individual, rather than something the man got through an acquired resistance to the drugs he was taking.
The vast pool of resistance mutations means the strain of HIV in question is resistant to many of the most common HIV medications, including Isentress (raltegravir), Vitekta (elvitegravir), Tivicay (dolutegravir), Ziagen (abacavir), Viread (tenofovir), Epivir (lamivudine), and Emtriva (emtricitabine). However, Poz's Benjamin Ryan reported that "despite all these resistance mutations, the man in the case study is currently on successful HIV treatment, with a fully suppressed viral load. He is taking Tivicay (dolutegravir), Prezcobix (darunavir/cobicistat), and Edurant (rilpivirine)."
So how do we know the man was really adherent to PrEP guidelines? Researchers gathered his pharmacy records, which showed he had consistent prescription refills. Liquid chromatography-mass spectrometry "was performed on the untimed plasma sample from day 0" to determine the quantities of each medication in his system. Dried blood spot testing collected on day 16 showed consistent dose-taking in the preceding one to two months, thus overlapping with the time period when he would have seroconverted to HIV-positive.
In addition, standard population sequencing and deep sequencing to 2 percent of the viral population was completed on day 7, as was phenotypic testing for resistance to integrase inhibitors, and "phylogenetic analysis of the V3 loop of envelope protein gp120" to characterize the "founder virus."
Knox and his fellow researchers told conference attendees that "to our knowledge, this is the first reported case of breakthrough HIV infection with evidence of long-term adherence to [Truvada as PrEP]."
There is further testing this individual could undergo. But further analysis seems unwarranted after the litany of tests the newly-poz man has already undergone. Moreover, if PrEP is 99 percent effective, this guy could indeed be that 1 percent. While none of the nearly 10,000 people in the famed iPrEx study of PrEP among gay and bi men and trans women acquired HIV -- and mutation like this wasn't seen among the participants -- scientists have always argued there could be a very small possibility of such.
While resistance to tenofovir is cited as a main concern among people living with HIV who are resistant to treatment worldwide, tenofovir-resistant strains of HIV only account for about 1 percent of all cases. Resistance to Truvada's other active ingredient, emtricitabine, is more common, but the strain that managed to bypass the safety of PrEP and infect the man in this study involved a mutation that was resistant to both medications, an exceedingly rare occurrence.
While this case proves that there is no 100 percent guarantee when PrEP is concerned, most experts, including those in this study, say that cases such as this will likely remain rare.