CONTACTAbout UsCAREER OPPORTUNITIESADVERTISE WITH USPRIVACY POLICYPRIVACY PREFERENCESTERMS OF USELEGAL NOTICE
© 2025 Equal Entertainment LLC.
All Rights reserved
All Rights reserved
By continuing to use our site, you agree to our Privacy Policy and Terms of Use.
We need your help
Your support makes The Advocate's original LGBTQ+ reporting possible. Become a member today to help us continue this work.
Your support makes The Advocate's original LGBTQ+ reporting possible. Become a member today to help us continue this work.
A sophisticated scanning technique can track the progression of HIV and could lead to new treatment options and the development of the next generation of anti-HIV drugs, scientists said on Friday. Positron emission tomography scans are usually used to identify cancerous tumors, but researchers believe the technology could play an important role in the battle against AIDS by identifying the impact of the virus on lymph nodes that could be treated with radiotherapy or surgery. The lymph nodes are believed to be major HIV reservoirs that can evade the effects of anti-HIV medications. C. David Pauza and scientists at the University of Maryland Biotechnology Institute in Baltimore took whole-body PET scans of 15 HIV patients and found fairly distinct sites of immune response during different stages of the illness. "We believe that if we identify those sites clearly during HIV infection, we encourage people to consider these types of interventions," Pauza said, referring to surgery or radiotherapy. During early disease, lymph nodes in the head and neck were activated, according to the PET scans, but in later stages the virus stimulated an immune response in areas of the torso and later in the bowel. HIV disease is currently treatable only with antiretroviral drugs. Surgery or radiotherapy would open up a new approach to the illness that has affected 42 million people worldwide. "We are not aware that it has ever been tried," said Pauza, who reported his findings in The Lancet. "We think it is appropriate to consider these approaches and also appropriate to learn from the cancer models because cancer is a disease of chronic cell activation and growth, and in some ways--even though HIV is triggered by a virus--it has some similarities." In cancer patients, PET scans measure the activity of cancerous cells, while in HIV it picks up levels of immune system reaction. David Schwartz and Sujatha Iyengar, of the Johns Hopkins University Bloomberg School of Hygiene and Public Health who also used PET scans to track HIV progression, said lymph node removal could give patients an opportunity for a break in antiretroviral treatment. "Although many systemic sites from which latent virus could be reactivated would be left, reactivation might not occur for months or years after removal of the active nodes, thereby allowing extended interruption of treatment," Schwartz wrote in a separate study published in The Lancet.
From our Sponsors
Most Popular
Bizarre Epstein files reference to Trump, Putin, and oral sex with ‘Bubba’ draws scrutiny in Congress
November 14 2025 4:08 PM
True
Jeffrey Epstein’s brother says the ‘Bubba’ mentioned in Trump oral sex email is not Bill Clinton
November 16 2025 9:15 AM
True
Watch Now: Pride Today
Latest Stories
Tucker Carlson and Milo Yiannopoulos spend two hours spewing homophobia and pseudo-science
December 04 2025 4:47 PM
'The Abandons' stars Gillian Anderson & Lena Headey want to make lesbian fans proud
December 04 2025 4:38 PM
Tig Notaro is working on a 'hot lesbian action' movie with Zack Snyder
December 04 2025 4:36 PM
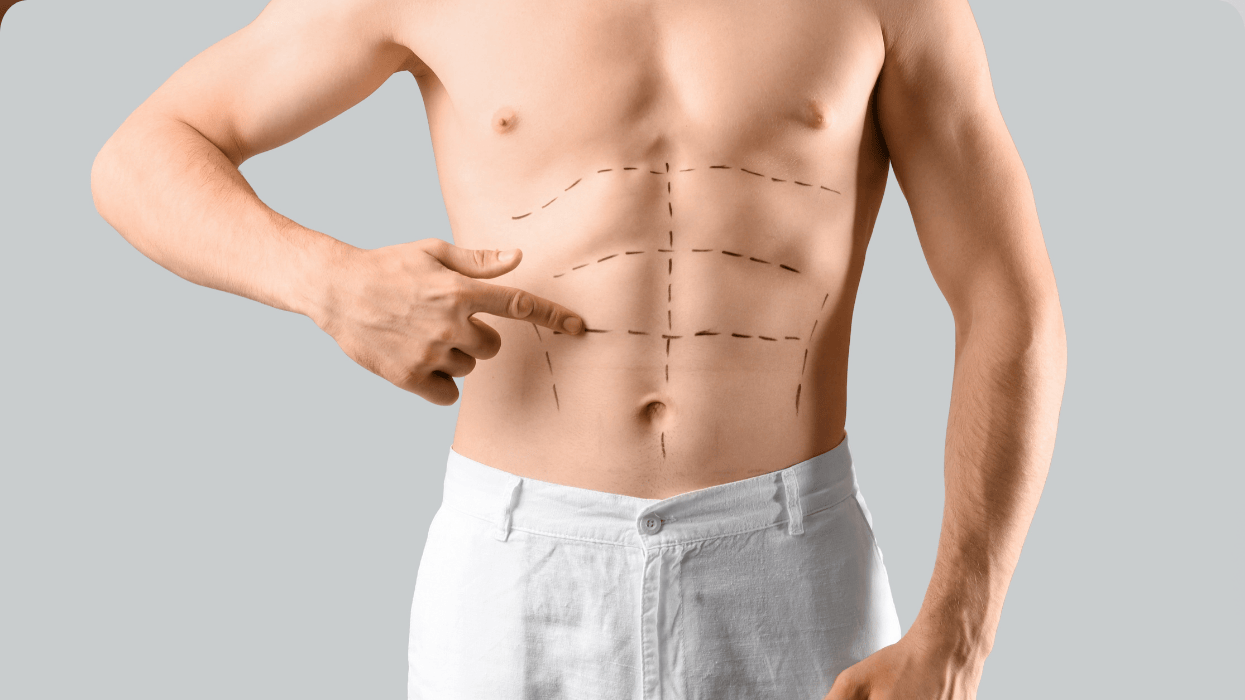
Cis men love top surgery—it should be available for all
December 04 2025 4:35 PM
Denver LGBTQ+ youth center closed indefinitely after burglar steals nearly $10K
December 04 2025 12:57 PM
Trans pastor says she’s ‘surrounded by loving kindness’ after coming out to New York congregation
December 04 2025 11:13 AM
Lesbian educator wins $700K after she was allegedly called a ‘witch’ in an ‘LGBTQ coven’
December 04 2025 10:59 AM
Years before Stonewall, a cafeteria riot became a breakthrough for trans rights
December 04 2025 10:50 AM
Charlie Kirk’s widow set to join out CBS News chief Bari Weiss for televised town hall
December 04 2025 10:20 AM
Women's Institute to ban transgender women after U.K. Supreme Court ruling
December 03 2025 4:10 PM
Grindr supports age verification bill introduced by two Republicans
December 03 2025 3:30 PM
Sarah Paulson & Holland Taylor's cutest moments on the Walk of Fame
December 03 2025 3:25 PM































































Charlie Kirk DID say stoning gay people was the 'perfect law' — and these other heinous quotes