CONTACTAbout UsCAREER OPPORTUNITIESADVERTISE WITH USPRIVACY POLICYPRIVACY PREFERENCESTERMS OF USELEGAL NOTICE
© 2025 Equal Entertainment LLC.
All Rights reserved
All Rights reserved
By continuing to use our site, you agree to our Privacy Policy and Terms of Use.
We need your help
Your support makes The Advocate's original LGBTQ+ reporting possible. Become a member today to help us continue this work.
Your support makes The Advocate's original LGBTQ+ reporting possible. Become a member today to help us continue this work.
This year I attended the 49th Interscience Conference on Antimicrobial Agents and Chemotherapy. More than 10,000 physicians, researchers and other health care professionals from around the globe gather each year at ICAAC to exchange the latest information and present research on topics related to HIV and other infectious diseases.
There was some interesting data presented on HIV and aging. Currently 15%-20% of HIV-positive individuals in the United States are over the age of 50. It's estimated that by 2015 this number will reach 50%.
What does this sharp rise in older HIV-positive individuals mean?
As the HIV population ages, we will begin to see more issues with brain disorders -- specifically Alzheimer's disease and dementia -- bone diseases like osteoporosis, and diabetes, kidney disease, and non-AIDS-related cancers.
A greater demand will be placed on services for older people with HIV, and this will likely burden the health care system, which is currently not equipped to handle these patients. Also, toxicities associated with long-term antiretroviral therapy will impose greater risks for comorbid conditions and premature death. Some HIV treatment advocates consider aging and HIV the number 1 issue and believe this topic deserves greater attention. Other health care providers, like myself, argued that the good news is that people with HIV are living longer.
There was a considerable amount of discussion regarding the expansion of HIV testing. In 2006 the Centers for Disease Control and Prevention recommended routine optional HIV testing for all adults who sought medical care, including those who visited emergency rooms. The majority of people who opted out of testing stated they did not believe they had any risk factors for acquiring HIV.
Researchers at George Washington University in Washington, D.C., tested discarded blood samples of emergency room patients who opted out of testing to calculate their HIV rate. Washington has the highest HIV prevalence in the United States -- at least 3% among people over 12 years old -- and the HIV-positive population is predominantly African-American.
Their results concluded that those individuals who declined HIV testing had an HIV rate more than two times higher than those who agreed to the testing.
The researchers believe that "it is critical for public health issues to determine whether the opt-out population is truly HIV-negative or whether their personal risk is being underestimated."
From our Sponsors
Most Popular
Bizarre Epstein files reference to Trump, Putin, and oral sex with ‘Bubba’ draws scrutiny in Congress
November 14 2025 4:08 PM
True
Jeffrey Epstein’s brother says the ‘Bubba’ mentioned in Trump oral sex email is not Bill Clinton
November 16 2025 9:15 AM
True
Watch Now: Pride Today
Latest Stories
Lesbian federal worker pleads for answers about wife trapped in immigration detention limbo
December 16 2025 5:08 PM
Michigan Republican U.S. Senate candidate Mike Rogers surrounds himself with hardcore LGBTQ+ rights opponents
December 16 2025 2:53 PM
True
Florida city installs Pride bike racks after being forced to remove rainbow crosswalks
December 16 2025 2:21 PM
Ariana Grande and Jonathan Bailey in talks to star in West End musical
December 16 2025 12:26 PM
Netflix's 'Boots' is canceled: Stars react to the heartbreaking news
December 16 2025 11:37 AM
How this Minnesota city redefined LGBTQ+ rights 50 years ago
December 16 2025 11:25 AM
Gen Z women are more likely to identify as bisexual but still embrace lesbian label: study
December 16 2025 11:10 AM
Is Texas using driver's license data to track transgender residents?
December 15 2025 6:46 PM
Rachel Maddow on standing up to government lies and her Walter Cronkite Award
December 15 2025 3:53 PM
Beloved gay 'General Hospital' star Anthony Geary dies at age 78
December 15 2025 2:07 PM
Rob Reiner deserves a place in queer TV history for Mike 'Meathead' Stivic in 'All in the Family'
December 15 2025 1:30 PM



















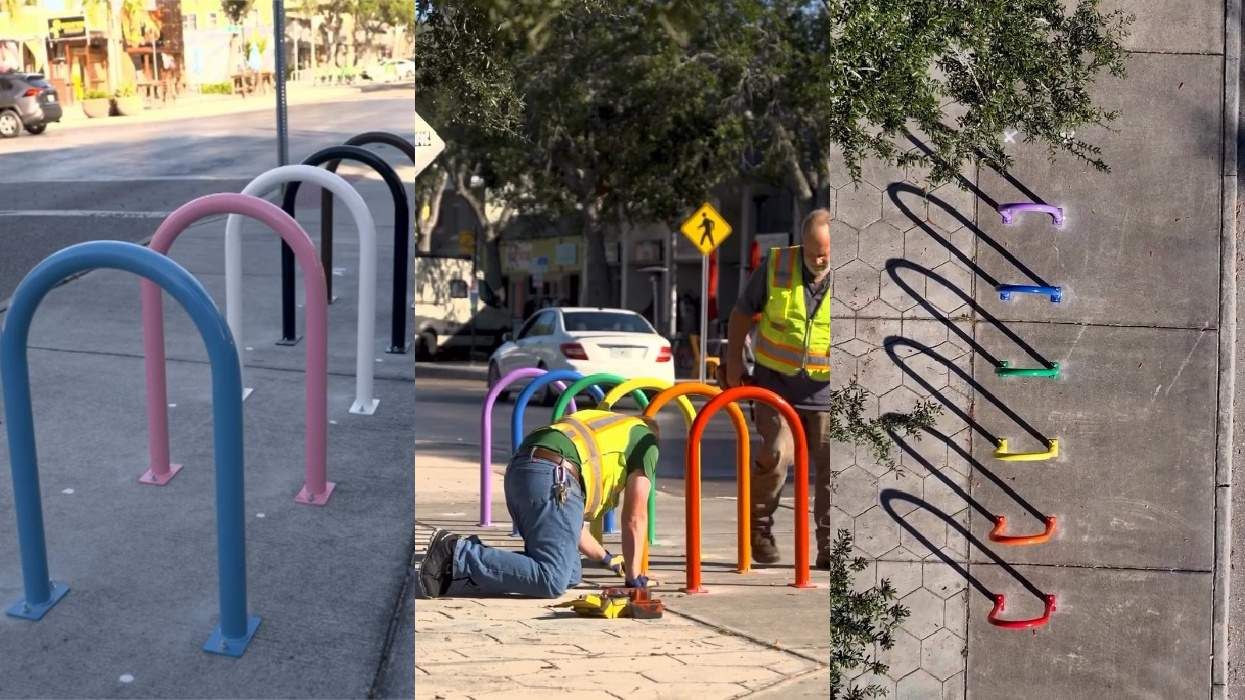















































Charlie Kirk DID say stoning gay people was the 'perfect law' — and these other heinous quotes