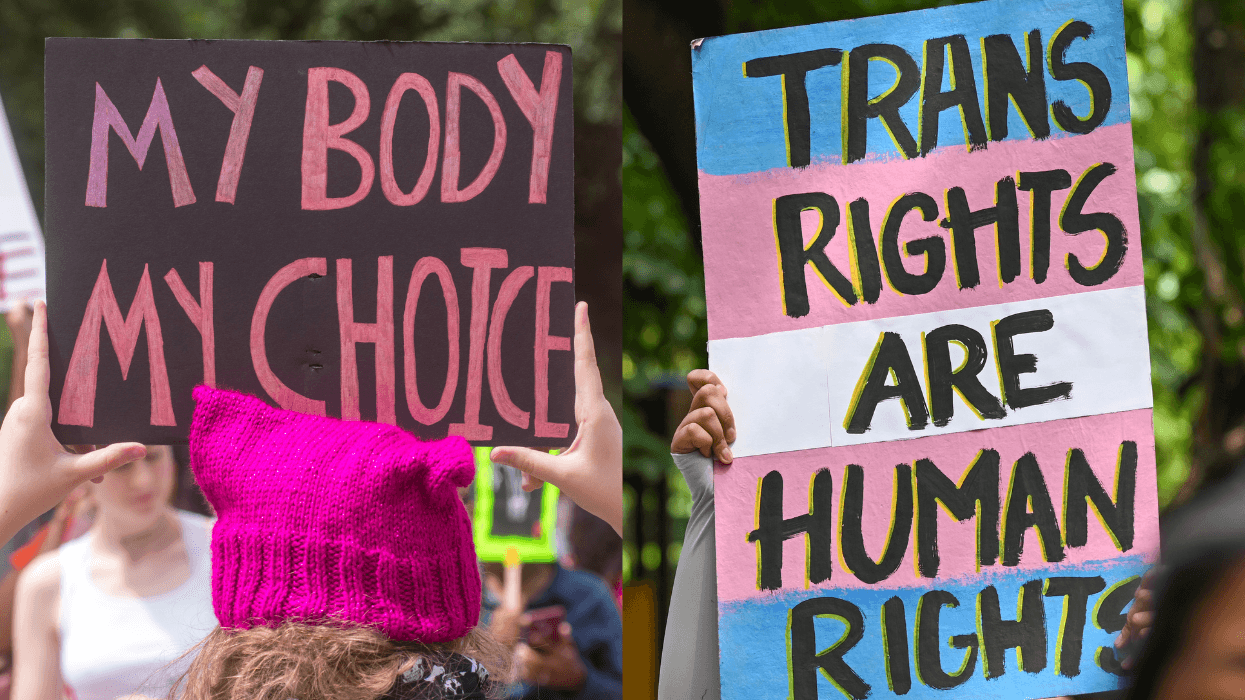South Carolina's supreme court has ordered Fortis Insurance to cough up $10 million for wrongly revoking coverage of a 17-year-old college student after he tested positive for HIV.
It is the most an insurance company has ever been ordered to pay in a case involving the practice of rescission -- when an insurance company retroactively cancels coverage based on alleged misstatements, often right after diagnoses of life-threatening diseases.
Chief Justice Jean Hoefer Toal (pictured) called the 2002 decision by Fortis Insurance "reprehensible."
The court upheld a lower court's ruling against Fortis. That court awarded Jerome Mitchell $15 million in punitive damages -- the supreme court reduced that amount by $5 million.
Mitchell first learned that he was HIV-positive when, while en route to college, he donated blood. Fortis then rescinded his policy, citing a note from a nurse in his medical records that suggested he might have been diagnosed prior to his obtaining his insurance policy.
An underwriter working for Fortis who was concerned they might not have a case wrote the following to a committee reviewing Mitchell's policy: "Technically, we do not have the results of the HIV tests. This is the only entry in the medical records regarding HIV status. Is it sufficient?"
His concerns were apparently ignored.
Insurance Co. Drops HIV Poz Teen, Pays Up