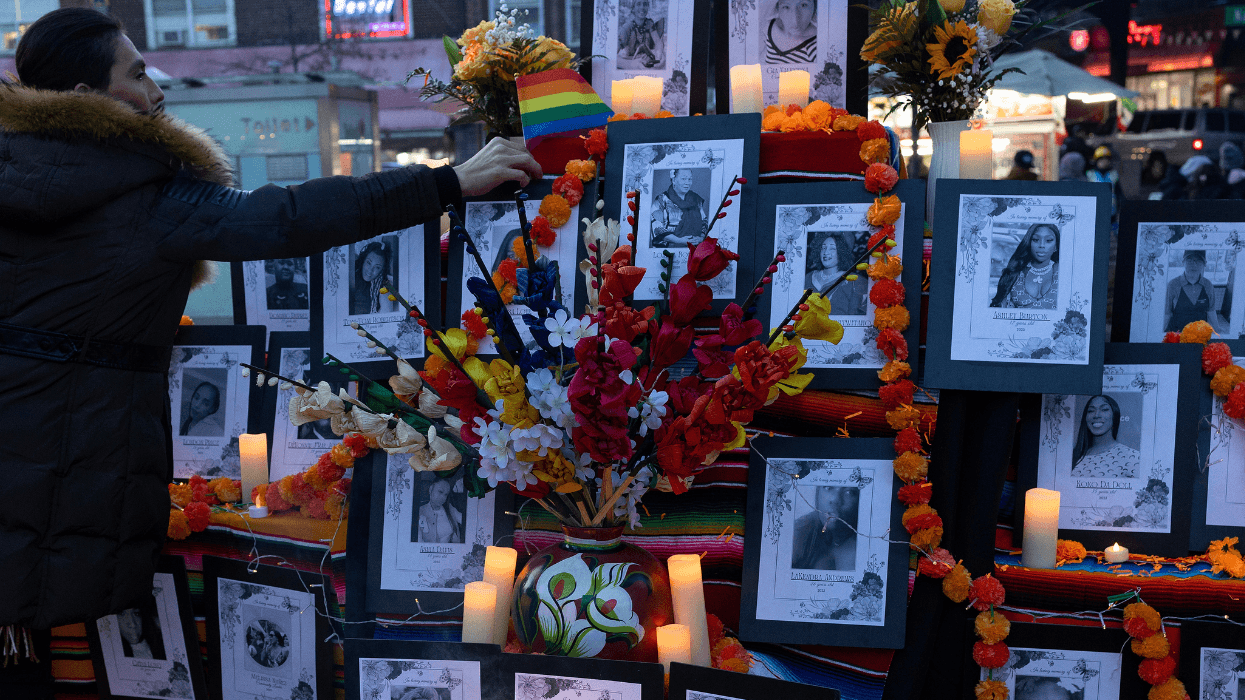A December report by the Centers for Disease Control says that an estimated 27 percent of transgender women are HIV positive, and that HIV prevalence for transgender women is nearly 50 times as high as for other adults.
In a New York City study, more than 90 percent of newly diagnosed trans women were African-American or Latino, and more than half were in their 20s.
But what accounts for these catastrophic numbers?
For one, the behaviors the report lists are like an encyclopedia of oppression and its outcomes, including "drug and alcohol abuse, sex work, incarceration, homelessness, attempted suicide, unemployment, lack of familial support, violence, stigma, and discrimination, limited health care access, and negative health care encounters."
It's a cycle that's been outlined by transgender activist Dean Spade and others: a young trans woman will be kicked out of her home by unaccepting parents, and, because her legal identity is still male, she would be barred by appropriate shelters and services. Experiencing homelessness and societal stigma, employment is often unattainable.
"When trans women aren't able to find jobs because of direct or indirect discrimination," Transgender Law Center attorney Sasha Buchert says, "they turn to street economies to feed themselves and to pay for the health care they need, and street work often places trans people at greater risk of contracting HIV and violence, especially for trans women of color who face racism, sexism and transphobia."
Societal prejudice toward trans women is still widespread, affecting access to housing, education and employment. The report notes that trans women are more likely to live in transient housing than other populations, and to be less educated.
The health care system itself can prove unwelcoming. While HIV-positive trans women are as likely to have health care coverage as other HIV-positive people, trans women are less likely to be on antiretroviral therapy. Buchert believes education on the part of care providers could improve this condition.
"Social service agencies could help by becoming more competent in working with transgender clients," she says. "Often, rather than enduring the stigmas they face at such places, trans women will simply forego the assistance, and miss the opportunity to check their HIV status or learn tools to reduce the likelihood of obtaining the virus."
This is, in part, because of the way that HIV prevention services are structured, according to Jaxon Mitchell, an HIV Prevention Specialist with the Cascade AIDS Project.
"Historically, HIV prevention and sexual/reproductive health services in general, have been organized by gender," Mitchell says. "For trans folks, gendered spaces almost always carry social and structural barriers. HIV prevention and testing services geared toward women frequently fall under the greater umbrella of reproductive health, which lacks the cultural competency to attend to the needs of trans women and carries many additional barriers."
In an almost nauseating twist to all this terrible news, it seems that law enforcement is compounding the problems of young transgender women by profiling them as sex workers, and seeing possession of condoms on their part as evidence of criminal activity, rather than precaution against the disease that's crippling their community.
This practice, which is being carried out in New York City and elsewhere, contradicts legal precedent, says Buchert.
"This use of condoms as per se evidence of illegal activity has already been struck down by the Supreme Court as a violation of privacy in Griswold v. Connecticut, which involved the use of condoms as evidence to prosecute for using contraception in 1960," Buchert says. "[The practice] is likely a constitutional violation of privacy, and it is an unconscionable public health hazard to use condoms as the basis of evidence of illegal activity. The impact of prosecuting individuals based on possession of a condom can only have a chilling effect the use of protection, and will create a larger public health threat for everyone, and especially for transgender women."
The CDC's report also details a "high-impact prevention approach" to reverse the trends it found. Some of the work begins with providing support to community groups that distribute condoms, conduct HIV testing, and operate referral networks and services. The CDC also announced plans to update the National HIV Surveillance System, the program to which new diagnoses are reported, so that transgender people are better identified within it.
The CDC says it will also award grants to researchers to develop new HIV prevention interventions, like the Life Skills program aimed at trans women aged 16 to 24, and Girlfriends, which targets adult trans women. In addition, the organization gives financial rewards to groups that provide effective HIV prevention to "young transgender people of color and their partners" for more than five years.
Given the CDC's history of ignoring or misclassifying transgender women in its data, however, Mitchell is skeptical about these new programs' likelihood for success.
"For years, transgender women have been misclassified as MSM, or Men Who Have Sex With Men, which has created a situation where trans folks in general have not been counted," Mitchell says.
The CDC's funding relies on research, which can create a loop in which trans women are always excluded.
"Without broad research demonstrating what we all know empirically -- that HIV infections among trans women, especially trans women of color, are unconscionably high -- funding for programs designed to meet trans women's unique needs will never be a priority."
LEELA GINELLE is the communications and development intern for TransActive Education and Advocacy.