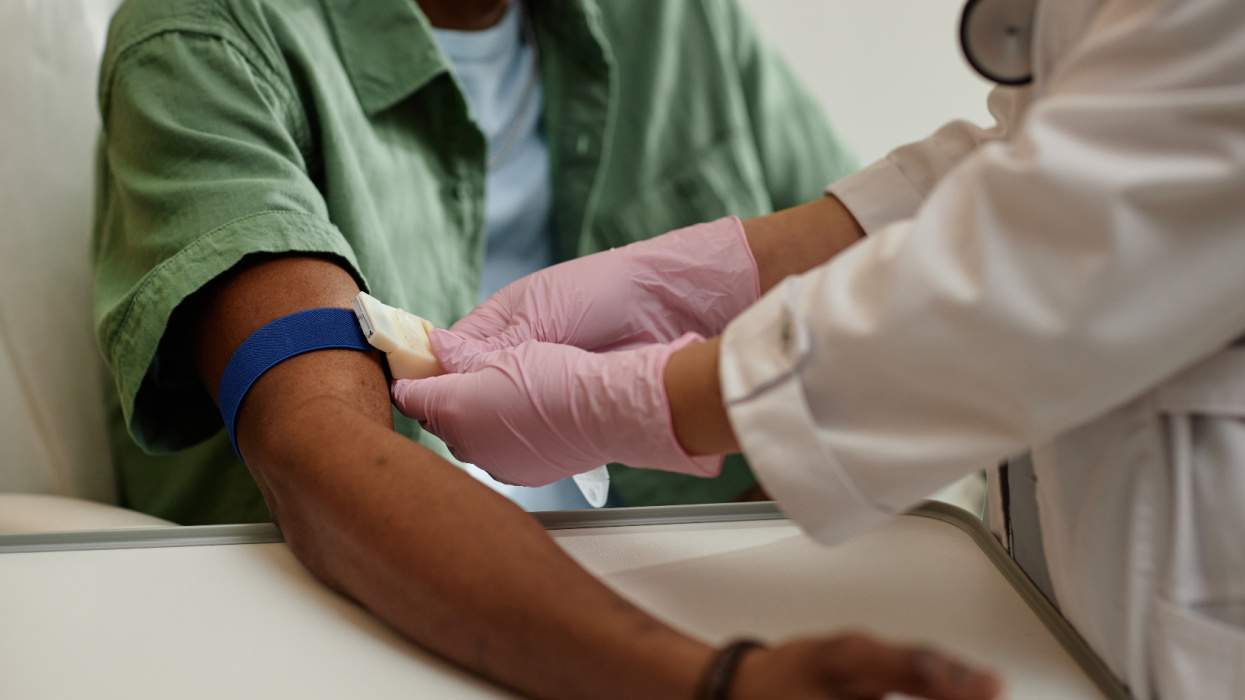
New guidelines released by federal and AIDS groups to help physicians and other health care professionals incorporate HIV prevention into primary health care include urging caregivers to ask detailed questions about sex-related and injection drug-related behaviors. Screening patients for risky behaviors and following up those screenings with reinforcement of safer-sex and safer-injection messages are the keys to bringing prevention-for-positives efforts into primary health care, according to the groups that formed the guidelines, which include the Centers for Disease Control and Prevention, the Health Resources and Services Administration, the National Institutes of Health, the HIV Medicine Association of the Infectious Diseases Society of America, and the HIV Prevention in Clinical Care Working Group. The guidelines are published in the January 1 issue of Clinical Infectious Diseases. "Behavioral change can be facilitated by environmental cues in the clinic or office, messages delivered to patients by clinicians or other qualified staff on-site, or referral to other persons or organizations providing prevention services," the group writes in the journal. "All patients should receive printed information about HIV transmission risks and preventing transmission of HIV to others." HIV-positive patients might also benefit from prevention case management, the authors write, which includes "intensive, client-centered risk assessment; prevention counseling; and assistance accessing other services to address issues that affect patients' health and ability to change risk-taking behavior." The guidelines were drafted as part of the CDC's shift in HIV prevention priorities to emphasize programs urging HIV-positive people to protect others from the virus. As much as $90 million in federal HIV prevention money has been diverted from traditional HIV prevention programs aimed at keeping HIV-negative people from becoming infected to prevention-for-positives initiatives.
Search
AI Powered
Human content,
AI powered search.
Latest Stories
Stay up to date with the latest in LGBTQ+ news with The Advocate’s email newsletter, in your inbox five days a week.
@ 2026 Equal Entertainment LLC.
All rights reserved
All rights reserved
By continuing to use our site, you agree to our Privacy Policy and Terms of Use.
The Latest
Support Independent Journalism
LGBTQ+ stories deserve to betold.
Your membership powers The Advocate's original reporting—stories that inform, protect, and celebrate our community.
Become a Member
FOR AS LITTLE AS $5. CANCEL ANYTIME.
More For You
Most Popular
@ 2026 Equal Entertainment LLC. All Rights reserved